
MANAGING DIABETES
The diabetes puzzle

Have a closer look at how different parts of your body can contribute to the progress of type 2 diabetes.
It can feel like there’s a countless number of things that can contribute to your diabetes health. This can make it hard to know where to focus and how all the information fits together. An easier way to process some of the facts may be to think of your body as a 7‑piece puzzle.
Let’s take a closer look at each puzzle piece to better understand what is happening in your body when you have type 2 diabetes.
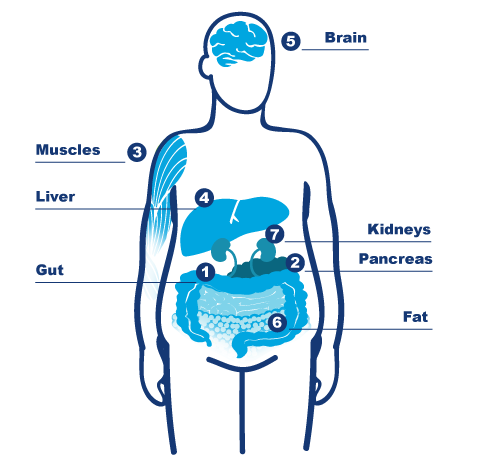
1. Gut
The gut is made up of organs like your stomach and intestines. When you eat, incretins (hormones such as glucagon-like peptide-1 [GLP-1] and gastric inhibitory peptide [GIP]) are released to help the body use glucose from the meal as well as suppressing your body's glucose production. With type 2 diabetes, there is a decreased incretin effect due to a lack of GLP-1 and resistance to the action of GIP in the body. This results in less insulin and increased blood glucose.

2. Pancreas
The pancreasPancreasA large organ behind the stomach. The pancreas not only makes pancreatic juices, or enzymes, to help the body digest food, but it also makes hormones such as insulin and glucagon, which are important for glucose metabolism. is where insulinInsulinA hormone made by the beta cells in the pancreas that helps glucose move from the blood into the cells. Insulin is also an injectable medicine that is used to treat diabetes by controlling the level of glucose in the blood. is made. Insulin helps control blood glucoseBlood glucoseThe main sugar found in the blood, and the body’s main source of energy. by moving glucose from the bloodstream into the body's cells for energy. The pancreas also makes the hormone glucagonGlucagonA hormone released by the alpha cells in the pancreas that helps release glucose stored in the liver when your blood glucose levels are too low. Glucagon is available in an injectable form and can be used to quickly raise blood glucose in severe hypoglycemia.. Glucagon tells the liver to release glucose into the blood to help balance blood glucose. With diabetes, the pancreas secretes less insulin and more glucagon, which can contribute to higher blood glucose.

3. Muscles
Your muscles get their energy from glucose. But with type 2 diabetes, insulin has trouble moving glucose into muscle cells. This is called insulin resistance. When the body does not have enough insulin in the blood, it means glucose cannot get into muscles to fuel them. Over time, the lack of glucose can lead to muscle cells dying, resulting in the loss of muscle mass.

4. Liver
If you have type 2 diabetes, your pancreas can release too much glucagon. This, in turn, causes the liver to release more glucose, leading to higher blood glucose levels.

5. Brain
A part of the brain called the hypothalamus helps regulate how much you eat, affects your body's sensitivity to insulin, and affects how your body metabolizes glucose and fats. In people with type 2 diabetes, changes in brain signaling can occur, resulting in less of a response from signals, such as insulin or GLP-1 levels, from the rest of the body.

6. Fat
Just like muscle cells and liver cells, fat cells can be insulin resistant if you are overweight and/or have type 2 diabetes. This can cause higher blood glucose levels. Healthy eating, staying active, and maintaining a healthy weight can help get rid of fat cells and may benefit you.

7. Kidneys
One job of the kidneys is to reabsorb blood glucose to help keep the energy that is stored from being lost. When you have type 2 diabetes, the kidneys reabsorb too much glucose back into the blood, making it hard to keep blood glucose levels under control.
When you understand how all 7 pieces of the puzzle work together, you have a more complete picture to help you manage your blood glucose. If you have any questions, be sure to ask your doctor.




